Shingles: Symptoms, Treatment and Prevention
This content is presented with the support of

Cassandre D.-S.-A., Christian P., Hugo D. & George M.
Change store
savings just for Moi!Enroll in
the program
Sign in
Access my Health Record, renew and pay for my prescriptions.
Sign inOffered by your Pharmacist Owners affiliated to Jean Coutu
Shop and enjoy Moi program offers and rewards.
This content is presented with the support of

Vaccination is the best way to protect yourself against shingles and its complications.
Nearly one in three people will develop shingles (herpes zoster) in their lifetime. Shingles can have a significant impact on the health and quality of life of those affected. Find out how to prevent and treat it.
Shingles is caused by the reactivation of the chicken pox virus. After an episode of chickenpox, this virus does not disappear completely: it remains dormant in certain nerve ganglia of the body. Years later, it can reactivate and cause shingles. Anyone who has had chickenpox can develop shingles.
This reactivation of the chickenpox virus can be triggered by a weakened immune system caused by:
The first symptoms of shingles often appear even before the rash. Many people first feel pain or a burning sensation in a specific area of the skin on one side of the body.
Early symptoms of shingles may include:
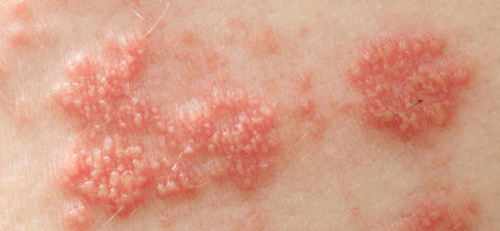
A few days later, a rash characteristic of shingles usually appears. It manifests itself as small red blisters clustered together, most often on the trunk or back, but sometimes also on the buttocks, limbs, face, or scalp.
Without treatment, shingles lesions take about three weeks to heal.
Although the virus can strike anyone who has had chickenpox, certain people are at greater risk of developing it:
Shingles is not directly contagious, in the sense that a person with shingles cannot transmit shingles to someone else. However, a person with shingles can transmit chickenpox to someone who has never had it before if that person comes into direct or indirect contact with the fluid in the lesions.
It is therefore important to wash your hands thoroughly to prevent contamination from person to person. In certain situations, it may be wise to avoid contact with the infected person, such as for pregnant women, newborns and people with weakened immune systems.
The most common complication of shingles is persistent nerve pain, known as post-herpetic neuralgia. It is caused by nerves being damaged by the virus attack. This consequence occurs in approximately 50% of people with shingles.
Often described as feeling like an “electric shock,” this pain is sometimes described as unbearable. It can last weeks, months, and in some rare cases, years or even a lifetime. Pain is sometimes accompanied by insomnia, fatigue, depression and social withdrawal.
Some other complications of shingles are possible but less common, such as loss of vision or hearing, facial paralysis, and secondary skin infections.
Shingles is unpredictable. It is impossible to know who will or will not develop these complications after having the virus. For this reason, it is very important to do everything possible to prevent it and to act quickly if symptoms appear. The sooner shingles is treated, the lower the risk of severe symptoms and complications.
In the event of symptoms that may indicate shingles, it is important to consult a doctor or pharmacist as soon as possible. Under certain conditions, your pharmacist may prescribe an antiviral medication to treat the infection quickly. Even if your pharmacist starts the treatment, you should still see a doctor afterwards to confirm the diagnosis.
The earlier treatment is started, the lower the risk of severe shingles symptoms and complications.
Acute episodes of shingles are treated with antiviral drugs, since it is a virus. To be most effective, they must be taken as soon as the first symptoms of shingles appear. Their main effects are to speed healing, reduce acute pain and lower the risk of post-shingles neuralgia.
In the event of acute pain during an episode of shingles, your doctor may prescribe or suggest the use of an analgesic.
If you suffer from post-shingles neuralgia, your doctor may prescribe pain management treatment in the form of oral, topical or injectable medication. These drugs generally require a doctor's prescription.
Your pharmacist can help you manage your pain and adjust your medication as needed.
Combined with medical treatment, shingles requires gentle, protective care to promote healing and scarring.
Avoid :
Vaccination is the best way to reduce the risk of developing shingles and its complications, such as post-shingles neuralgia. It also reduces the severity of symptoms if the virus decides to manifest itself anyway, and reduces the risk of recurrence in people who have already had shingles.
The following people can be vaccinated against shingles:
In Quebec, shingles vaccination is free for people aged 71 and over and for immunocompromised adults. Eligibility criteria to receive it for free are different for other Canadian provinces. The shingles vaccine is generally covered by private insurance plans for people who are not eligible to receive it for free.
You can get a shingles vaccination right at the pharmacy. Your pharmacist or nurse can assess your vaccination needs and administer the vaccine under certain conditions. For more information on shingles, talk to your pharmacist.
You may change the store at any time.